Leaves of three, leave them be. This is a great reminder for most varieties of poison ivy and oak. However there are other plants dissimilar to the triad-leaf type that can cause a similar effect as the most common culprits of what we call contact dermatitis.
In the United States, the most infamous plant offenders belong to the genus Toxicodendron, which means 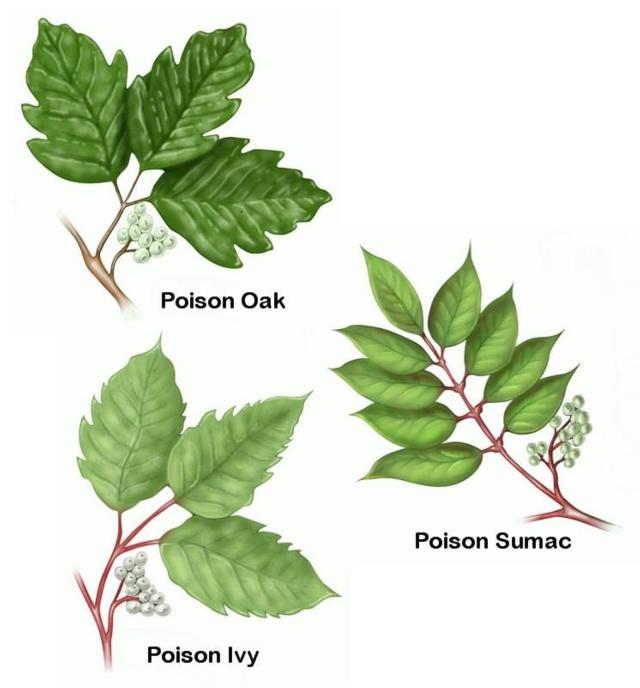 "poisonous tree." (1) These include several varieties of poison ivy, oak, and sumac. This species of plant can be found throughout the country and affects those of every race, age, and skin type.
"poisonous tree." (1) These include several varieties of poison ivy, oak, and sumac. This species of plant can be found throughout the country and affects those of every race, age, and skin type.
Get The Latest News!
Don't miss our top stories and need-to-know news everyday in your inbox.
Lucky for some of us, it seems that as we get older our sensitivity to the plants decreases.
About 50 percent of people react to poison ivy in nature, although even more than that react with allergy testing. (2)
Poison ivy and similar plants are composed of a blend of compounds that form a colorless oil that can get on one's skin, clothes, tools, pets, among other things. The exposure can be more severe if the plant is broken or bruised, such as when cutting weeds or a recent rainfall.
The plant oil is very strong and even a single exposure can be enough to cause the ensuing itchy rash.
It shows up initially on the skin that was directly exposed to the plant. Once the plant oil is washed off the skin, it cannot spread to other people. New poison ivy skin lesions can develop at different times based on the amount of plant oil exposure and the thickness of the skin in the area affected, giving the impression that the rash is "spreading."
Often we inadvertently re-expose ourselves by touching poison ivy-contaminated tools, pet fur, clothes, or oil that resided under our fingernails. In those cases, our close contacts can then develop the rash.
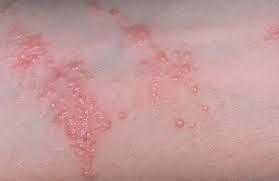 The detestable poison ivy rash usually begins 1-2 days after exposure and is very itchy and red. The rash can consist of both large and small bumps and in worse cases, vesicles can develop.
The detestable poison ivy rash usually begins 1-2 days after exposure and is very itchy and red. The rash can consist of both large and small bumps and in worse cases, vesicles can develop.
Avoiding poison ivy and the like is often tricky but can be helped by wearing protective clothing and heavy duty vinyl gloves (latex/rubber gloves are not protective enough).
Poison ivy oil is stable even at high temperatures so burning it may cause particles to be dispersed in the air.
Once exposed, be sure to remove contaminated clothing and wash thoroughly with soap and water as soon as possible. The longer the oil is on the skin, the more likely one will develop a rash from it. (3)
Tecnu, a chemical inactivator found over the counter, and Dial ultra dishwashing soap have both been found effective to reduce dermatitis severity associated with poison ivy. (4) But these need to be used shortly after exposure to be effective.
Items that have come in contact with the plant also need to be washed in warm, soapy water.
Left untreated, poison ivy rash typically resolves on its own in a few weeks. But it can be extremely aggravating in the interim. A potential complication is a secondary bacterial infection such as with Strep or Staph species.
General measures to treat poison ivy rash include cool, wet compresses and oatmeal baths.
Your health-care provider may prescribe a medium to high potentcy steroid cream. These cannot be applied to the face or genitals though.
In severe cases, steroids taken orally, such as prednisone, are indicated. Oral steroids do carry side effects and have some drug interactions, however, and so these need to be discussed with your health care provider.
Michele Brannan is a certified Physician Assistant of Internal Medicine and has been in practice in the River Bend area for over 10 years.
The health information provided herein is not intended to replace the advice or discussion with a healthcare provider and is for educational purposes only. Before making any decisions regarding your health, speak with your healthcare provider.
REFERENCES:
1. Crawford GH, McGovern TW. Poison ivy. N Engl J Med 2002; 347:1723.
2. Baer RL. Poison ivy dermatitis. Cutis 1990; 46:34.
3. McGovern TW, Barkley TM. Botanical dermatology. Int J Dermatol 1998; 37:321.
4. Stibich AW, Yagan M, Sharma V, et al. cost-effective post-exposre prevention of poison ivy dermatitis. Int J Dermatol 2000; 39:515.
More like this:

